Ministry : Ministry of Health and Family Welfare
Aims to reduce the financial burden on poor and vulnerable groups arising out of catastrophic hospital episodes and ensure their access to quality health services.
Scheme:
- PM-JAY is a scheme of the government under Ayushman Bharat.
- PMJAY is government-sponsored health insurance scheme, that will provide free coverage of up to Rs 5 lakh per family per year in any government or empanelled private hospitals all over India.
- It will cover beneficiaries families identified on the basis of Socio Economic Caste Survey (SECC) 2011 in 444 districts of 30 states/Union Territories.
- National Health Agency (NHA) is the apex body for implementing this scheme.
- States will be required to form State Health Agency (SHA) to implement scheme and at the district level also structure for its implementation will be set up.
- Around 13000 hospitals both public and private in the country have been coordinated for implementation of the scheme.
- PMJAY will be funded with 60% contribution from Centre and remaining from the states.
- NITI Aayog will be working as partner for this scheme for operationalizing robust, modular and interoperable IT platform which will involve a paperless and cashless transaction.
- PMJAY is entitlement based scheme with entitlement decided on basis of deprivation criteria in the SECC database.
- There will be no cap on family size and age under this scheme.
- The benefit cover under it also includes pre and post-hospitalisation expenses.
- It also takes into consideration all pre-existing medical conditions.
- It will provide reimbursement for bed charges and drugs and diagnostics two days before, during and 15 days after hospitalisation. Beneficiary will be also paid transport allowance for hospitalisation defined under it.
- The payment for treatment will be done on package rate which will be defined by Government in advance basis.
- The package rates will include all costs associated with treatment.
- States and UTs have flexibility to modify these rates within limited bandwidth.
- PMJAY allows national portability i.e. resident of any part of country is entitled for free hospitalization at empanelled hospital anywhere in the country.
- It will strengthen healthcare services in India by targeting poor and vulnerable population of the country.
- The scheme allows beneficiary to take cashless benefits from any public or private empanelled hospitals across the country.
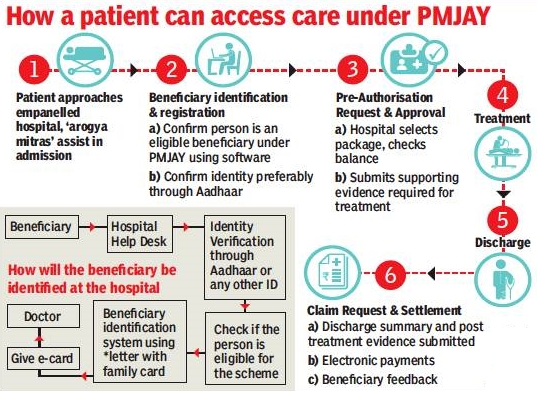
- ID documentation required for verifying beneficiary under this scheme may be Aadhaar card or election ID card or ration card.
- Aadhaar is not mandatory.
- Beneficiaries will QR codes having letters for verification through scanning.
- Scheme also seeks to accelerate India’s progress towards the achievement of Universal Health Coverage (UHC) and Sustainable Development Goal – 3 (SDG3).
National Health Agency converted to National Health Authority:
“National Health Agency” has been dissolved and it is now restructured as an Authority to effectively the implement Pradhan Mantri – Jan Arogya Yojana (PM-JAY).
The National Health Authority would be empowered with full autonomy, accountability and the mandate to implement PM-JAY through an efficient, effective and transparent decision-making process by aligning the accountability with responsibility.
Why the Authority has been constituted?
The reasons for restructuring as an authority are:
- To enable faster decision-making.
- Replacing the multi-layered structure with a simplified structure.
- Authority will be able to specify treatment protocols and enforce their compliance.
- The Authority with a stronger mandate would be able to prevent, detect and control frauds, abuse and redress grievances, thus resulting in the reduction of leakages.
The National Health Authority would be chaired by Union Health Minister and have representation from the Government and domain experts.